Recently updated on January 20th, 2026 at 12:02 pm

Medication management is a critical component of treatment in the field of mental health. It involves the careful selection, dosing, and monitoring of medications prescribed to treat mental health conditions. This process is essential because it ensures that patients receive the most effective therapeutic benefits while minimizing potential side effects.
Psychiatric medication management can dramatically enhance the quality of life for individuals with mental health disorders, fitting seamlessly into broader treatment plans that may include therapy, counselling, and lifestyle adjustments.
Here is a complete guide to effective medication management mental health patients need:
The Significance of Medication Management for Mental Health:
The significance of medication management in treating mental health conditions cannot be overstated. This practice is crucial for stabilizing mood, reducing symptoms of mental illness, and enhancing overall functioning, thereby providing a stable foundation for comprehensive mental health treatment.
For numerous patients, medication is not merely an aspect of their treatment strategy but a fundamental component that enables significant therapeutic progress. It allows individuals to gain the mental clarity and emotional stability necessary for engaging more effectively in psychotherapy sessions and for implementing vital lifestyle changes. These changes are often essential for long-term recovery and well-being, helping patients to rebuild their lives and maintain their health over time.
By improving core symptoms through medication, patients are better positioned to focus on recovery and personal growth, making it a pivotal part of holistic mental health care. You can see many mental health influencers emphasizing the importance of medication management for mental health.
Common Types of Psychiatric Medications:
Psychiatric medications are indispensable tools in the management of various mental health conditions, each tailored to address specific symptoms and disorders through distinct mechanisms:
- Antidepressants: These medications, including Selective Serotonin Reuptake Inhibitors (SSRIs) and Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs), are primarily prescribed for depression and anxiety disorders. SSRIs, like fluoxetine and sertraline, increase serotonin levels in the brain, which can improve mood and emotional stability.
SNRIs, such as venlafaxine and duloxetine, target both serotonin and norepinephrine, helping to elevate mood and possibly improve energy levels and concentration. Antidepressants can take several weeks to show effects, but they are key in managing daily function and improving life quality.
- Antipsychotics: Used to treat conditions like schizophrenia and bipolar disorder, antipsychotics can reduce or alleviate symptoms such as hallucinations, delusions, and severe mood swings.
These medications, such as risperidone and olanzapine, work by influencing various neurotransmitters in the brain, including dopamine. The goal is to reduce the intensity of symptoms and prevent relapses of severe episodes.
- Mood Stabilizers: These medications are crucial in treating mood disorders, particularly bipolar disorder. Mood stabilizers, including lithium and valproic acid, help prevent the dramatic highs (mania) and lows (depression) associated with bipolar disorder.
By maintaining a more stable mood, these drugs allow individuals to function more consistently and reduce the risk of harm from extreme mood states.
Potential Benefits of Effectively Managed Medication

Effectively managed psychiatric medications offer several transformative benefits that significantly enhance daily functioning and overall quality of life for individuals with mental health disorders:
- Symptom Reduction: Proper medication management can dramatically reduce the symptoms of mental health disorders. For instance, antidepressants can alleviate feelings of overwhelming sadness or hopelessness in depression, allowing individuals to feel more stable day-to-day.
- Improved Daily Functioning: Medication effectively controls symptoms, helping individuals perform daily tasks more efficiently. Someone with controlled symptoms is better able to focus at work, engage in social activities, and maintain personal relationships.
- Enhanced Quality of Life: With symptoms managed, patients often experience an overall improvement in quality of life. They are more likely to enjoy activities, pursue interests, and maintain social contacts that might have been neglected during periods of unmanaged mental health.
- Support for Other Treatments: Medications can provide the necessary mental stability for patients to benefit from other therapies, such as psychotherapy or counselling, thereby enhancing the effectiveness of comprehensive mental health care.
Common Side Effects and the Importance of Communication
While psychiatric medications are beneficial, they are not without risks. Managing side effects through ongoing communication with healthcare providers is crucial:
- Range of Side Effects: Medications can cause a variety of side effects, such as weight gain, sleep disturbances, and sometimes more severe effects like changes in blood sugar or cholesterol levels. Antipsychotics, for example, can lead to metabolic syndrome, while SSRIs may cause sexual dysfunction.
- Monitoring and Management: Regular check-ups with a healthcare provider help monitor side effects and adjust medication doses as necessary. This proactive approach helps manage side effects before they become severe.
- Open Communication: Patients need to have open lines of communication with their healthcare providers. Discussing any new symptoms or changes in overall health can help adjust treatment plans promptly and effectively.
- Empowerment through Information: Educating patients about potential side effects and when to report them empowers them to take an active role in their treatment. This knowledge helps them manage their health proactively and communicate effectively with their healthcare team.
Additionally, polypharmacy—managing multiple medications—is a common challenge in elderly care, increasing the risk of adverse drug events. Deprescribing unnecessary medications, especially sedatives and benzodiazepines, is a key strategy to minimize falls and other side effects, balanced with patient preferences and quality of life considerations.
Collaborative Approach in Medication Management
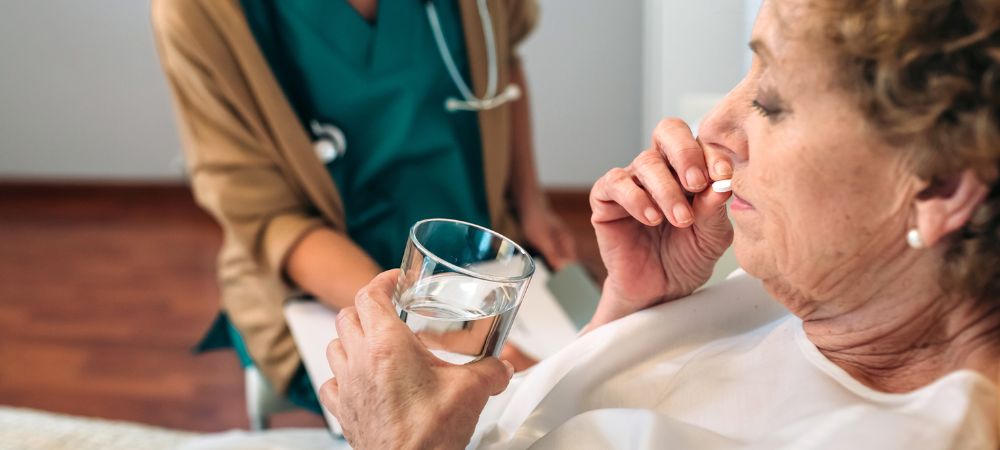
A collaborative approach in medication management involves multiple healthcare professionals working together to optimize treatment outcomes for patients with mental health issues:
- Team Involvement:Medications can cause a variety of side effects, such as weight gain, sleep disturbances, and metabolic changes. For elderly patients, clinical decision support systems and Beers Criteria help flag potentially inappropriate medications, notably CNS drugs like antipsychotics and benzodiazepines, with routine monitoring for specific risks such as hyponatremia and QTc prolongation.
- Tailored Treatment Plans: Each patient’s treatment plan is customized based on their unique needs and circumstances. This personalized approach ensures that the medication regimen is optimized for the best possible outcomes, considering factors like other medical conditions and personal preferences.
- Dynamic and Responsive Care: As patients progress or encounter challenges, the healthcare team remains flexible, adjusting treatment plans in response to changes in mental health status and overall well-being. This dynamic approach helps to ensure that care remains effective over time.
- Regular Monitoring: Regular assessments by the healthcare team help track the effectiveness of the medication and make adjustments as needed, ensuring that the treatment continues to meet the patient’s evolving needs.
In geriatric mental health, treatment plans are highly personalized based on comorbidity profiles, frailty, and patient goals. The ‘5 R’s’ framework—right person, medicine, dose, time, and route—guides therapy, supported by regular medication reviews that often lead to persistent changes, improving safety and outcomes.
Addressing Common Myths and Stigma
Efforts to dispel myths and reduce stigma around psychiatric medication are essential in mental health care:
- Challenging Misconceptions: Common myths include the belief that psychiatric medications are addictive or merely “mind-altering.” It’s important to educate people that these medications adjust chemical imbalances in the brain, similar to how diabetes medication regulates insulin.
- Understanding Medication Needs: Another widespread misconception is that using psychiatric medications is a sign of weakness or a failure to manage problems on one’s own. It is vital to communicate that these medications are often necessary for stabilization and can be critical for recovery.
- Promoting Scientific Backing: Education should emphasize that medication management is based on rigorous scientific research, making it a valid and often essential aspect of mental health treatment.
- Encouraging Open Dialogue: By fostering open discussions about psychiatric medications, healthcare providers can help reduce stigma and promote a more accepting attitude toward mental health challenges.
Practical Advice for Patients
For patients on psychiatric medications, adherence to their treatment regimen is crucial for success:
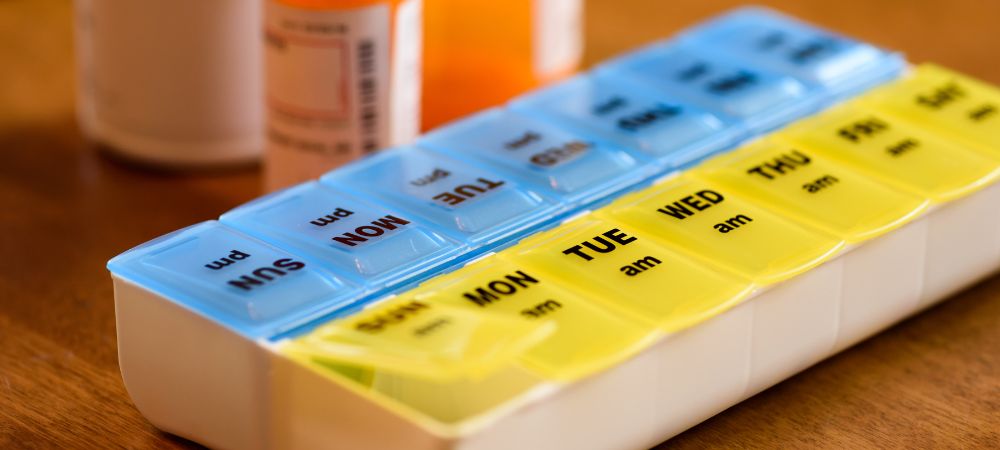
- Utilizing Tools: Employing daily medication organizers and digital reminder apps can help patients maintain their medication schedules accurately. These tools prevent missed doses and help keep treatment on track.
- Maintaining Routines: Establishing and sticking to a daily routine can enhance medication adherence, making it easier for patients to remember their medications as part of their daily activities.
- Regular Healthcare Visits: Regular check-ups with healthcare providers are crucial. These visits allow for the assessment of the medication’s effectiveness and the adjustment of dosages or medications as necessary to optimize treatment. You can also sign up for senior care in home services.
- Engagement in Treatment: Patients are encouraged to be actively engaged in their treatment plans, discussing any concerns and observations with their healthcare providers. This helps them fine-tune their medications in response to any side effects or changes in their condition.
Recent innovations in digital health, such as smart pill dispensers, telehealth platforms, and wearable devices, are increasingly adopted to support medication adherence and monitor side effects in real-time. These tools help bridge gaps in care coordination and empower patients and caregivers, though technology access remains a consideration for some seniors.
FAQs:
The Bottom Line:
Medication management is more than just taking pills; it’s a comprehensive approach to ensure that individuals receive optimal benefits from their psychiatric medications. By understanding the types of medications, their potential benefits and side effects, and the importance of a collaborative healthcare approach, patients can better navigate their treatment options.
If you are seeking effective medication management for your elderly loved ones, contact Loving Homecare. Our team is dedicated to providing tailored support that respects the unique needs of each patient, ensuring their safety, well-being, and improved quality of life. Reach out to us today to learn how we can help manage and optimize your loved one’s medication regimen.

